Dementia care homes with specialised nutrition programs in the UK (and how to staff them well)
In UK dementia care homes, nutrition is never “just the food.” It’s hydration, dignity, routine, safety, and one of the most reliable ways to improve day-to-day wellbeing. As the Royal College of Nursing puts it, “Mealtimes are fundamental to health and quality of life.” (The Royal College of Nursing)
That’s why more dementia care homes are building specialised nutrition programs—not “special diets,” but practical, person-centred systems that help residents eat and drink well even as needs change. And crucially, these programs only work when the kitchen is staffed by chefs and kitchen teams who understand dementia-friendly catering.
If you’re a care provider looking for a chef (or a full kitchen team) with dementia experience, HCC-Temps Staffing Agency supports UK care homes with reliable, trained catering staff. You’ll find more details at hcctemps.co.uk.
What “specialised nutrition” really means in dementia care homes
The Alzheimer’s Society notes that “People with dementia often experience problems with eating and drinking.” (Alzheimer’s Society) Those problems can include reduced appetite, forgetfulness, sensory changes, difficulty using cutlery, or swallowing issues (dysphagia). So the best dementia nutrition programs focus on supporting eating, rather than restricting it.


The British Dietetic Association (BDA) warns against overly strict food rules: “It is crucial to avoid restrictive diets for patients with dementia.” (British Dietetic Association) In practice, that often means prioritising enjoyment and intake—while still managing clinical risks with professional guidance.
The core building blocks of a strong dementia nutrition program
Here’s what high-performing dementia care homes in the UK commonly build into their nutrition and hydration approach.
1) Nutrition screening + clear care plans
Malnutrition risk is common in older adults. Age UK estimates “around one in ten” over-65s are malnourished or at risk in the UK. (Age UK)
Many care homes use BAPEN’s ‘MUST’ screening process—“a five-step screening tool to identify adults… malnourished [or] at risk of malnutrition.” (BAPEN) Screening is only useful if it leads to action, and NICE is explicit that people at risk should have a plan: “All people… at risk of malnutrition should receive a nutritional care plan.” (Clinical Knowledge Summaries)
Kitchen impact: chefs need to be able to follow nutrition care plans consistently—especially when intake dips or weight changes.
2) Dementia-friendly dining that increases intake
The RCN highlights how powerful good mealtime support can be: “Good mealtime care is transformational to the experience of people with dementia living in care homes.” (The Royal College of Nursing)
Common features include:
- Finger foods and “little-and-often” menus for people who wander or struggle to sit through meals
- High-contrast plates and simplified table settings (to reduce confusion)
- Familiar foods and culturally appropriate menus (comfort drives intake)
- Flexible meal times (when appetite is best, not when the rota says so)
Kitchen impact: dementia care homes benefit from chefs who can cook home-style, adapt presentation, and work closely with care staff.
3) Fortified foods and “food-first” energy/protein strategies
When appetite is low, portion size often needs to go down—but nutrition must go up. Many specialist programs rely on:
- Fortified mash/soups/sauces
- High-protein snacks and puddings
- Nourishing drinks between meals
Kitchen impact: this is where skilled care-home chefs shine—because fortification must still taste good, look appealing, and fit individual preferences.

4) Hydration that’s actively supported (not passively offered)
Dehydration risk rises with memory issues and reduced thirst cues. The RCN advises: “Encourage people to drink small amounts throughout the day.” (The Royal College of Nursing)
Specialised hydration programs often include:
- Drink rounds with choice and prompts
- Jelly/ice-lollies/fruit options for people who reject cups
- Hydration support at medication times
Kitchen impact: kitchens often own the beverage offer. A well-run kitchen can make hydration effortless, appealing, and routine.
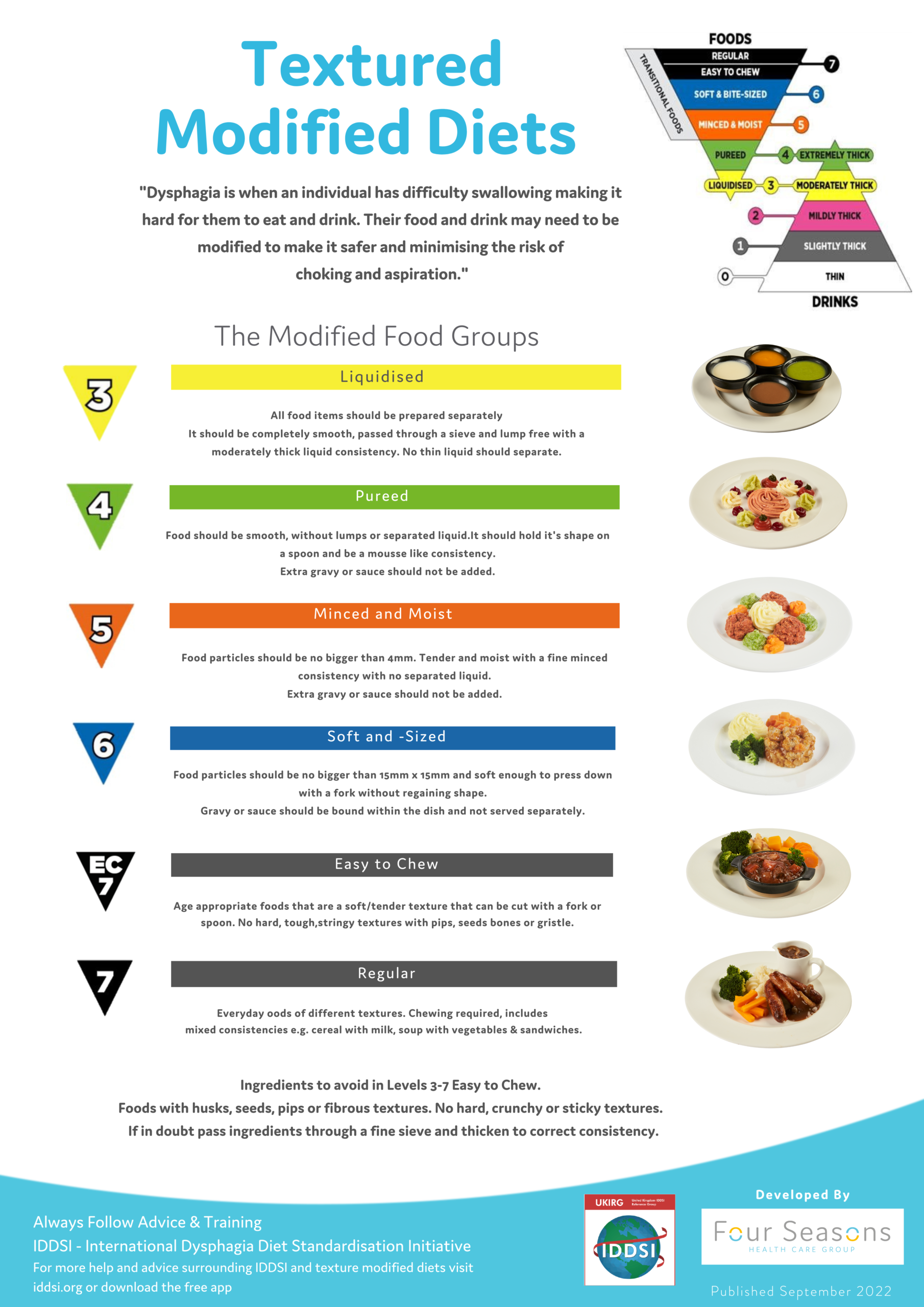
5) Texture-modified diets and dysphagia safety
Swallowing difficulties need specialist input. NICE states people with indicators of dysphagia “should be referred to… specialist training… for example speech and language therapists.” (NICE)
Many care homes align with speech and language therapy guidance and structured texture frameworks, then translate that into:
- Consistent texture-modified meals
- Safer thickened fluids where prescribed
- Clear kitchen labelling and cross-checks
Kitchen impact: texture modification is a skill. The right chef prevents risk while keeping meals enjoyable.
What care providers should look for when hiring a dementia care chef
If you’re recruiting for a dementia care home kitchen, use this quick checklist to find people who can deliver a specialist nutrition program—not just cook a menu.
Your dementia-friendly chef should be able to:
- Cook appetising soft/texture-modified meals without “puree plate boredom”
- Fortify meals to increase calories/protein without huge portions
- Work to nutrition care plans and respond quickly to intake changes
- Support finger foods, snack programs, and flexible meal services
- Communicate calmly with residents and collaborate with care staff
This is exactly where specialist staffing support helps.
How HCC-Temps Staffing Agency supports dementia care homes
Specialised nutrition programs succeed when the kitchen is stable, covered, and led by people who understand care environments. HCC-Temps Staffing Agency helps UK care homes source dependable chefs and kitchen staff—particularly where dementia-friendly catering, consistency, and compliance matter.
If your service is:
- Expanding dementia beds
- Upgrading to a more structured nutrition/hydration program
- Struggling with chef shortages, sickness cover, or last-minute cancellations
- Needing cooks confident with fortified meals and texture-modified diets
…then it’s worth speaking with a staffing partner who understands the pace and expectations of care catering.
To hire a dementia-experienced chef or kitchen team, visit hcctemps.co.uk and connect with HCC-Temps Staffing Agency.
Final thought: the best dementia nutrition programs are human programs
Guidance, screening tools, and care plans matter—but residents experience food emotionally: comfort, identity, and routine. When a care home invests in dementia-friendly dining and hires chefs who can deliver it consistently, nutrition becomes one of the strongest daily supports you can provide.
If you would like to discuss your kitchen staffing, then contact one of our team today – https://www.hcctemps.co.uk/contact/